Highlights
- Ethnic minorities are less likely to receive continuous glucose monitors despite having higher diabetes rates.
- People from minority backgrounds make up 17.5 per cent of populations in areas with below-average device prescribing.
- Ethnicity and deprivation account for up to 77 per cent of variance in diabetes technology prescribing.
People from ethnic minority backgrounds in England have significantly less access to vital diabetes technology, despite being at greater risk of developing the condition, according to groundbreaking research.
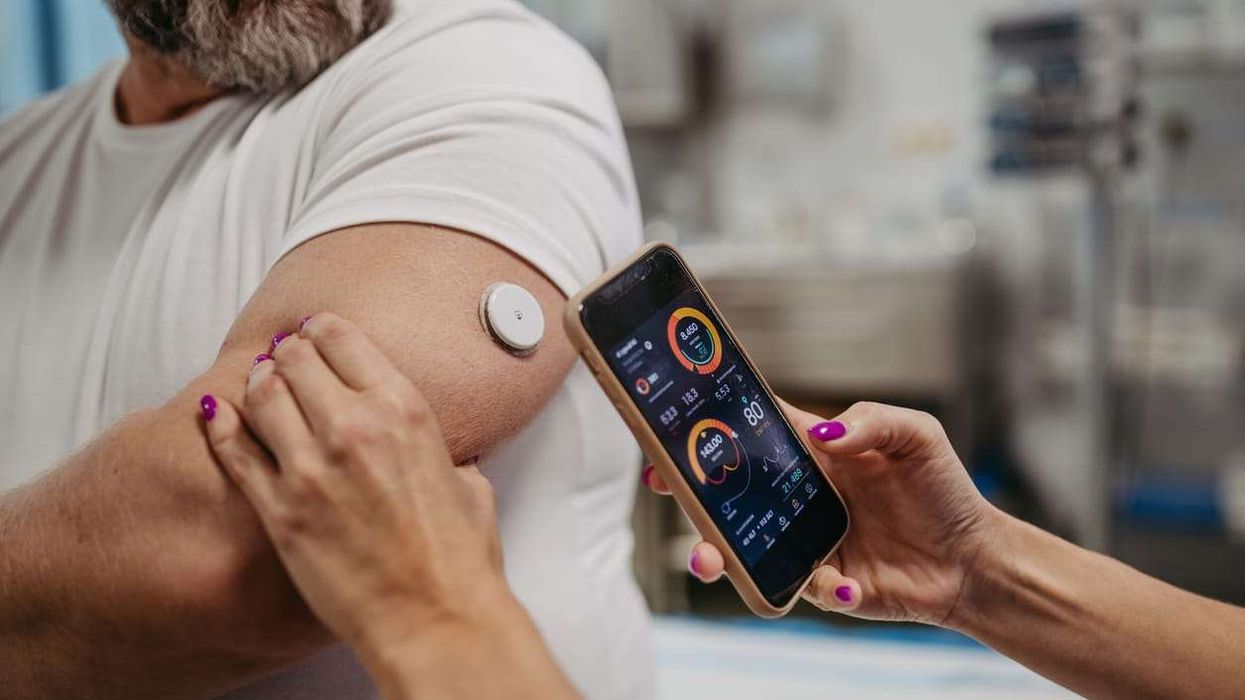
The study, published in Diabetic Medicine, reveals that black and south Asian communities face significantly lower prescribing rates for continuous glucose monitors (CGMs) – devices that help people manage their blood glucose levels more effectively than traditional finger-prick tests.
Analysis shows that ethnic minorities represent 17.5 per cent of the population in integrated care boards (ICBs) with below-average CGM prescribing rates in 2024. In contrast, they comprise just 5.3 per cent of populations in ICBs with above-average prescribing rates.
Professor Samuel Seidu, lead author from the University of Leicester, described the findings as the "first national analysis in England to demonstrate, with robust prescribing data, that significant ethnic inequalities exist in access to continuous glucose monitoring across both type 1 and type 2 diabetes".
The disparity is particularly concerning as approximately 5.8 m people across the UK live with diabetes, with black and south Asian communities facing heightened risk of developing type 2 diabetes by age 25.
Call for urgent action
Professor Seidu noted that ethnicity and deprivation together account for up to 77 per cent of variance in CGM prescribing for type 2 diabetes, indicating that "structural inequities are deeply embedded" in the healthcare system.
Despite National Institute for Health and Care Excellence (NICE) guidelines stating all adults with type 1 and 2 diabetes should have access to diabetes technology including CGMs, implementation remains inconsistent across England.
Anthony Walker, policy lead at Diabetes UK, emphasised that "actively raising awareness among underserved communities is crucial" and called for healthcare professionals to be supported in identifying access gaps.
Diabetes advocate Daniel Newman, who has type 1 diabetes, stressed that "access to CGMs should be based on clinical need, not determined by postcode, ethnicity or income", urging that NICE guidance be "actively implemented for everyone who qualifies".
NHS England has been approached for comment on the findings.